Rabies
 Rabies is a viral infection that can be transmitted from animals to people. It is most commonly transmitted through saliva (spit) of an infected animal, usually after a bite. The disease attacks the nervous system and eventually affects the brain. Once symptoms appear, rabies is usually fatal.
Rabies is a viral infection that can be transmitted from animals to people. It is most commonly transmitted through saliva (spit) of an infected animal, usually after a bite. The disease attacks the nervous system and eventually affects the brain. Once symptoms appear, rabies is usually fatal.
Image Content Provider: CDC/Dr. Fred A. Murphy
On this Page
Symptoms
After contact with the rabies virus, symptoms typically take between 20 and 60 days to appear. Occasionally, symptoms take only days to appear, but sometimes they don't appear for years. There is often discomfort or pain at the site of a bite. Symptoms may also be flu-like and include fever, headache and weakness (general feeling of being unwell). As the disease progresses, an infected person may experience increased difficulty with swallowing, excessive salivating, muscle spasms and unusual behavior. Once a person begins to show signs of the disease, it is usually too late to treat it successfully and survival is rare.
Causes
Rabies is a viral infection usually transmitted to humans by a bite from an infected animal. Infected animals can include domestic pets (often stray cats or dogs), skunks, foxes, coyotes, wolves, raccoons and other biting mammals such as bats. Rabies can also spread when saliva from a rabid animal gets into a fresh cut, wound or intact mucous membranes such as the eye, nose or mouth. Rarely, rabies spreads in the air of caves infested with rabid bats. Children are at greater risk if not taught to avoid approaching a sick or dead animal out of curiosity.
Treatment
There is no specific treatment for rabies. A bite wound or scratch from a rabid animal must be washed thoroughly as soon as possible. It is critical to get medical attention within 24 hours if bitten or attacked by a domestic or wild animal, especially if the animal is acting strangely or seems sick. Immunization given after exposure to the virus (called post-exposure prophylaxis) can be effective at preventing rabies. A health care professional will decide what treatment to use.
Prevention
Pre-exposure vaccinations are available for individuals at high risk. These may include:
- biological and medical laboratory workers
- veterinarians
- animal and wildlife control officers
- hunters and trappers
- spelunkers (cave explorers)
- people travelling to areas with high numbers of rabies cases
Get medical treatment within 24 hours if bitten or scratched by a domestic or wild animal. Post-exposure vaccinations are available for those bitten by potentially rabid animals.
Pets should be vaccinated and their rabies immunizations kept up-to-date. Do not allow pets to roam freely outdoors, particularly at night. Avoid contact with wildlife and stray animals. Teach children never to approach unfamiliar or stray animals. Do not keep wild animals as pets. Report any strange acting or dead animals found on your property to the local public health unit or animal control office.
To report human exposure to an animal suspected of having rabies contact Health Links – Info Santé at 204-788-8200 in Winnipeg or toll-free 1-888-315-9257.
To report a domestic animal exposed to or injured by an animal suspected of having rabies (where no human exposure has occurred) contact Manitoba Agriculture at 204-470-1108.
Rabies Surveillance Data
Rabies is a reportable disease under the Health of Animals Act, the Public Health Act and the Animal Diseases Act and all suspect cases in animals and humans must be reported. All suspect cases of rabies are verified in a Canadian Food Inspection Agency rabies laboratory.
There have been no reported human cases of rabies on record in Manitoba.
Rabies Cases in Animals
The animal rabies dashboard is an interactive web page that displays all laboratory confirmed positive rabies results from animal exposures in Manitoba since 2014. It allows for quick navigation of results by year, species and region. The dashboard is updated quarterly to provide the most current surveillance information.
For surveillance data for animal cases of rabies in Canada see: CFIA Rabies in Canada.
Manitoba Health Resources
For the Public
- Rabies Fact Sheet
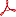
(July 2014) - The Community Dog Book
For Health Care Providers
- RE: Change in HyperRab Format - Update
January 10, 2020 - Report of Suspected Rabies Exposure: Letter to Health Care Professionals
(May 1, 2017) - Rabies: Protocol for Management of Human Rabies and Management of Exposures to Animals to Prevent Human Rabies
(December 2019 with February 2026 Updates) - Suspected Rabies Exposure and RPEP Report Form
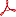
(January 2026)
Research Articles
Other Resources
- Public Health Agency of Canada - Rabies
- Public Health Agency of Canada - Rabies Virus - Pathogen Safety Data Sheet - Infectious Substances
- Centers for Disease Control and Prevention - Rabies
Communicable Disease Control (CDC)
Public Health
Manitoba Health
4th Floor - 300 Carlton St.
Winnipeg MB R3B 3M9 CANADA
Health Links – Info Santé
204-788-8200 or 1-888-315-9257


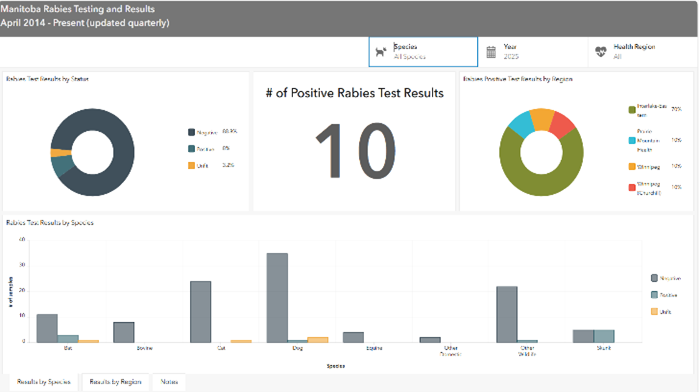 View the animal rabies dashboard
View the animal rabies dashboard
